Contents
ToggleWhat is Microscopy?
Microscopy is the term used for the practice of using a microscope. The microscope is an essential tool that is widely used by medical professionals, scientists and collectors to study objects that are too small to be seen clearly by the naked eye.

A microscope uses lenses to magnify small objects so that they may be observed closely to gain an understanding of the cellular structures and properties of the object.
Thy have helped mankind study a multitude of microscopic organisms that, despite being invisible to the naked eye, are all around us. For example, human body parts such as organs and other tissues are made of cells that can only be seen or studied using a microscope. Other living organisms such as bacteria and viruses that cause many diseases that affect the lives of everyone in the world, such as the SARS-CoV-2 virus which caused the Coronavirus disease (COVID-19), are also studied under the microscope.
Microscopes are used by scientists in many fields including animal and plant biology, environmental sciences such as geology and oceanography, and forensic science. They are also used in other activities such as jewellery, soldering, and coin and stamp collecting.
Microscopes are essential in cellular pathology
Since microscopes offer the ability to see tiny things in an incredible amount of detail, it’s not surprising that they are used by medical professionals to diagnose and treat diseases on a daily basis.
The two main categories of microscope used in clinical settings are the basic light microscope and the more advanced electron microscope. The most commonly used light microscope is the compound microscope.
The smallest visible object that can be seen by the human eye is less than 100 micrometres, and since animal cells range from 10 to 100 micrometres, the microscope is an essential tool in cellular pathology.
Biopsy Analysis
When a disease is suspected, a tissue specimen is regularly required in the process of deriving a diagnosis and confirming the presence of a disease state. This process begins with a biopsy, which can include a wide range of different techniques. Common biopsies include core biopsies from breast, prostate and renal tissue, as well as excision biopsies from the skin.
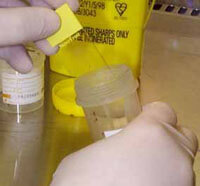
Once the biopsy has been removed, it is immediately placed into a specimen pot with a fixative, such as 100% formalin. The purpose of this measure is to preserve the cells in a life-like state. It achieves this in a variety of ways including prevention of autolysis, putrification, and maintaining antigenicity. It is then transported to the pathology laboratory for processing.
Prior to the specimen being placed into the cassette(s), the specimen dissection takes place. Typically, the areas of interest are sampled, and if applicable, the lymph nodes and tumor margins are also sampled as these can help guide treatment options and prognosis.
For example, if cancer cells are still remaining outside of the margin, further surgery may be required. Additionally, if cancer cells are discovered in the lymph nodes, this can indicate metastasis.
Although many samples warrant just a single cassette, there are often many cassettes per patient sample. Once labeled, cut and placed into their cassettes, they can be processed, which today is typically a heavily automated process.
In short, this involves a series of steps including tissue sample dehydration, clearing, embedding in paraffin wax and staining with a histological stain. Dehydration is an important step since the beginning stage i.e. formalin, is not miscible with the end stage i.e. paraffin wax.

Tissue sample dehydration involves the tissue being submerged in a series of graded alcohols to remove water e.g. 70%, 90%, and 100% ethanol. Once the dehydration process is complete, clearing is the next step, which removes the dehydrating agent e.g. ethanol, and replaces it with a solvent miscible with wax e.g. xylene.
The paraffin wax is crucial to the embedding process, which involves placing the tissue into a mold, and hot paraffin wax is then added and left until cool and solid. The specimen now embedded in wax can be efficiently cut into sections using an apparatus referred to as a microtome, and 4µm slices are the typical thickness for histological samples. The resultant and extremely delicate sections are immediately placed onto a water bath and then onto glass slides ready to be stained.
Haematoxylin and eosin (H&E) is the principal and routine stain used on all received samples, and the diagnosis of malignancies is based largely upon this procedure.
Additionally, there are many other stains, termed “special stains” that are utilized to identify other structures not possible with H&E. For example, silver stains are commonly employed as a connective tissue stain to identify and observe disturbed patterns of reticulin fibers in cirrhosis and some tumors.
Looking Through the Microscope
Once the patient sample has reached the final stage of tissue preparation, i.e. it has been microscopically prepared and stained, it is ready to be observed by a pathologist and the results reported.
There are 3 important questions asked of every specimen:
- What’s the diagnosis?
- What is the prognosis? and
- What is the resulting treatment?

In short, the diagnosis involves the clinician looking for any structural and morphological changes in the tissue, and checking if they fit with the data set. Furthermore, the pathologist will need to request further special staining if they can’t be sure with an H&E stain alone.
In addition to a diagnosis, the prognosis and treatment are also points of interest. For example, if neoplasia was observed, the pathologist would need to answer whether it was malignant or benign, as well as the grade, whether it was metastatic and provide potential treatment options.
Immunohistochemistry (IHC)
At approximately day 4, immunohistochemistry may also be employed for identification of a certain antigen in tissue by an antibody specific to that antigen. The site of antibody/antigen binding must then be labeled for microscopic visualization, and this technique is particularly useful for tumor typing, prognosis, and therapy.

Immunohistochemistry (IHC) is a technique which detects antigens in cells or tissue by utilizing the ability of antibodies to bind to specific antigens in biological tissues.
IHC staining is commonly utilized in the diagnosis of neoplasia. For example, specific molecular markers can be detected which are characteristic of a particular cellular event e.g. cellular proliferation or apoptosis of a particular tissue, helping to differentiate between a primary or a secondary tumor. Thus, common immunohistochemistry investigations include primary and secondary tumor typing and the confirmation of metastasis.
The visualization of the antibody-antigen interaction can be achieved in numerous ways. For example, the antibody can be conjugated to an enzyme such as peroxidase, which catalyzes a color-producing reaction. Additionally, there are other labels that can be conjugated to the antibody including enzyme-Horse radish peroxidase + Chromogen-Diaminobenzidine tetrahydrochloride (DAB), as well as fluorescent labels.
A good example of IHC utility in the diagnosis of neoplasia is the identification of specific markers for diagnosis, tumor typing, and confirmation of metastasis, which often involves the use of particular antibody panels. For example, a CK7, CK20, and TTF-1 antibody panel, which is useful in the diagnosis of lung tumors and for the differential diagnosis of primary pulmonary adenocarcinomas from extrapulmonary adenocarcinomas metastatic to the lung.
